The African continent has recorded a total of 3,682,261 confirmed cases of Covid-19, 95,591 deaths and 3,212,077 recoveries since the Covid-19 pandemic outbreak.
By early January 2021, COVID-19, caused by the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), had resulted in more than 83 million confirmed cases and more than 1·8 million deaths.
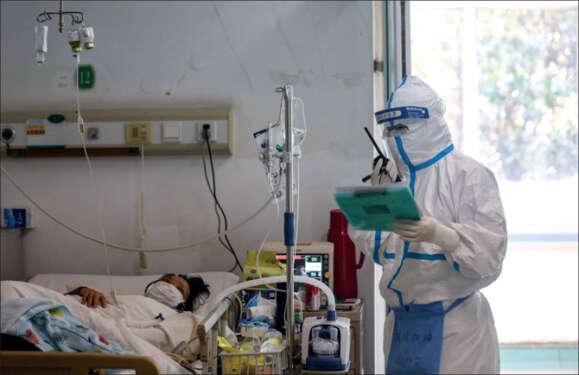
The clinical spectrum of SARS-CoV-2 infection is wide, encompassing asymptomatic infection, fever, fatigue, myalgias, mild upper respiratory tract illness, severe life-threatening viral pneumonia requiring admission to hospital, and death.
At the moment, 34.4 million Covid-19 tests have been conducted in Africa.
As much as we celebrate the high number of recoveries that continue to be recorded daily from various countries, there is a need to take care of those who have recovered from the virus.
Did you know that post-COVID-19 complications could be dire and fatal?
Well, the acting Director of the Ghana Infectious Disease Centre (GIDC), Dr Joseph Adjetey Oliver-Commey has come out to outline how fatal the complications could be.
According to Dr Oliver-Commey, post-coronavirus disease (COVID-19) clinics should be established to help manage the disease’s impact on patients who have recovered from it.
The clinics are meant to help the patients with lingering symptoms until they were deemed to be free, to an appreciable extent, from any complications.
Also Read: COVAX in Africa: Resetting the economy?
In an interview with a local daily in Chana, Dr Oliver-Commey urged all recovered patients who had tested negative but still had some lingering symptoms not to become complacent because they had recovered but pay attention to whatever symptoms might be lingering and report quickly to the hospital to avert complications and avoidable deaths.

“Patients would have recovered and tested negative, but the disease may have affected some internal organs, such as the lungs, brain, heart, kidneys and liver, causing them to still have symptoms of the disease,” he said.
Dr Oliver-Commey, who is also a member of the National COVID-19 Management Team, said the centre began undertaking post-COVID-19 clinics when it noticed that some recovered patients still exhibited symptoms, a situation referred to as long COVID.
“COVID-19 may leave scars in the lungs, making people affected unable to breathe normally as they did before, with the slightest thing they do making them gasp for breath.
“Meanwhile, all tests on them return negative, but you look at their CT scans and you find injury scars. So, yes, the recovery rate is high, but the effects of the virus can linger on and that is what we call post-COVID complication,” he said.
He said some post-COVID-19 complications could last for close to eight months, while some were irreversible.
He said the body could, after a while, adjust to the irreversible condition and the affected person would have to manage and live with it for the rest of his or her life.
Fortunately, he said, it was possible for health professionals to apply medication and guidance to reverse what was reversible over time.
Dr Oliver-Commey said most people infected with COVID-19 recovered completely within a few weeks, but others, with even mild versions of the disease, continued to exhibit symptoms after their initial recovery.
“Older people and people with serious medical conditions are the most likely to experience lingering COVID-19 symptoms. However, even young and otherwise healthy people can feel unwell for weeks to months after infection.
He said the most common signs and symptoms that lingered over time included fatigue, shortness of breath, cough, pain in the joints and chest pain.
Other long-term signs and symptoms included muscle pain or headache, fast or pounding heartbeat, loss of smell or taste, memory loss, lack of concentration, sleep problems, rashes and hair loss and, then, in the long term, organ damage, he said.
He said even though the COVID-19 was seen as a disease that primarily affected the lungs, it could damage many other organs as well.
Dr Oliver-Commey appealed passionately to the public to adhere strictly to the prevention protocols on the disease, such as wearing face masks, washing of hands and physical distancing.
He said those were currently the only sure ways to stay safe and avoid getting infected.
He said it was critical that the majority of the population wore masks at all times to break the transmission of the disease.
“The disease is transmitted through droplets from the mouth and nostrils but was not airborne and so the mask prevents us from inhaling the virus. We need also to wash our hands with soap under running water regularly since the hands pick the virus in the droplets in the atmosphere and introduce these into the body when we touch our faces, mouths, eyes and noses,” he said.
He advised that people who knew or suspected they had been exposed to the virus but were asymptomatic must report the symptoms they developed, even after the 14-day incubation period of the disease.
Physicians are observing persisting symptoms and unexpected, substantial organ dysfunction after SARS-CoV-2 infection in an increasing number of patients who have recovered, as previously observed in the SARS outbreak.
However, COVID-19 is a new disease and uncertainty remains regarding the possible long-term health sequelae.
This is particularly relevant for patients with severe symptoms, including those who required mechanical ventilation during their hospital stay, for whom long-term complications and incomplete recovery after discharge would be expected.
Unfortunately, few reports exist on the clinical picture of the aftermath of COVID-19.
The study by Chaolin Huang and colleagues in The Lancet is relevant and timely.
They describe the clinical follow-up of a cohort of 1733 adult patients (48% women, 52% men; median age 57·0 years, IQR 47·0–65·0) with COVID-19 who were discharged from Jin Yin-tan Hospital (Wuhan, China).
Six months after illness onset, 76% (1265 of 1655) of the patients reported at least one symptom that persisted, with fatigue or muscle weakness being the most frequently reported symptom (63%, 1038 of 1655).
More than 50% of patients presented with residual chest imaging abnormalities.
Disease severity during the acute phase was independently associated with the extent of lung diffusion impairment at follow-up (odds ratio 4·60, 95% CI 1·85–11·48), with 56% (48 of 86) of patients requiring high-flow nasal cannula, non-invasive ventilation, and invasive mechanical ventilation during their hospital stay having impaired pulmonary diffusion capacity.
These findings are consistent with those from earlier small studies that reported lingering radiological and pulmonary diffusion abnormalities in a sizeable proportion of COVID-19 patients up to 3 months after hospital discharge.
Evidence from previous coronavirus outbreaks suggests that some degree of lung damage could persist, as shown in patients who recovered from SARS, 38% of whom had reduced lung diffusion capacity 15 years after infection.
Although SARS-CoV-2 primarily affects the lungs, several other organs, including the kidney, can also be affected.