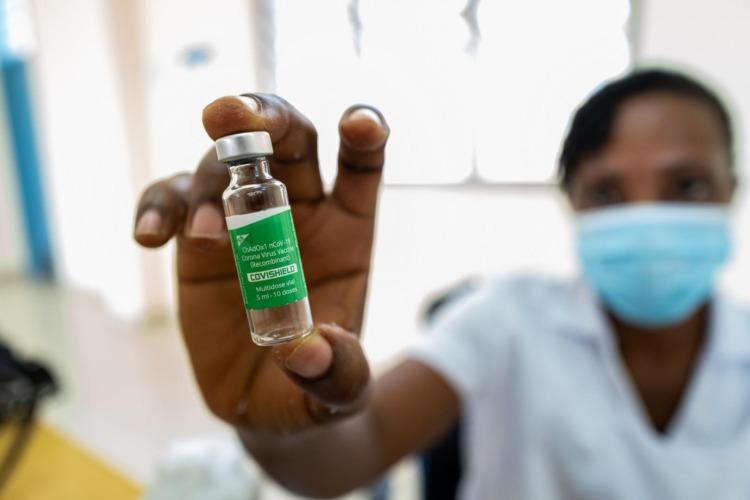
If the Pharmaceutical Manufacturing Plan for Africa that was recently adopted by the African Union is anything to go by, only few member states have strong regulatory authorities with the functions necessary to oversee the pharmaceutical markets.
Africa represents 14% of the world’s population, however, it only contributes to less than 0.1 per cent of world’s vaccine. According to data by the World Health Organisation, (WHO) there are fewer than 10 African manufacturers with vaccine production. These are based in five countries namely Egypt, Morocco, Senegal, South Africa and Tunisia. There is very limited upstream production with most local companies only engaging in packaging and labelling, and occasionally fill and finish steps. Noteworthy, there are about 80 sterile injectables facilities on the continent, which may provide an opportunity for vaccine production given the primary dosage form in Africa is vials.
How does that capacity affect vaccine availability in the continent?
Almost all the current vaccine capacity in Africa is focused on supply to internal country markets with very little export taking place. Current capacities are modestly scaled with a glaring absence of large-scale (fewer than 100 million doses) capacity.
As highlighted by COVID-19, this severely limits vaccine availability in disease emergency situations as there is no immediate readiness to repurpose facilities for large-scale production through partnerships. It is therefore vitally important that African vaccine manufacturers establish supply networks to export to markets (in Africa and elsewhere). Supply chain could use the existing economic zones in Africa. For example, the Economic Community of West African States.
Should Africa consider self-sufficiency in production?
Absolutely! Look at the recent global pandemic and its effects on the continent’s preparedness with regard to vaccines and health protective gears to combat and contain the pandemic. The continent heavily relied on vaccines imported from India and China. Most African countries are supplied with vaccines by UNICEF supported by Gavi, the Vaccine Alliance, with fewer than 10 countries being self-sufficient in terms of vaccine procurement. This has led to a very specific shaping of vaccine markets in Africa where more than 1.5 billion doses are supplied through UNICEF.
Consequently, this presents enormous challenges when trying to establish sustainable vaccine industries in Africa which would ideally require advance purchasing support from African governments. In the current dispensation this is simply not possible when most countries don’t buy their own vaccines and therefore cannot commit to buying locally manufactured vaccines.
So what are the challenges to achieving this production in Africa?
According to an analysis by WHO, one of the biggest impediment is the way vaccine markets are structured in Africa. Without the commitment and support to buy vaccine manufactured in Africa it will forever remain a difficult challenge to build a sustainable industry capable of producing vaccine doses at scale.
This is where African governments, continental bodies such as the African Union and other stakeholders can make a difference. The current system design requires a shift and complete review to enable this desperately needed capacity to be established as shown by COVID-19 and the delays despite the best efforts of the COVAX Facility.
Vaccine manufacturing is complex and requires huge financial investments and a long-term vision.
There is a need to focus core issues such as innovative financing, enabling local and regional regulatory capacity to assure quality, critical technical elements including skills development, technology transfer and product development partnerships, Good Manufacturing Practice facility design and establishment.
Kenya’s strategic response to the vaccine production crisis.
Kenya’s journey towards human vaccines self-sufficiency through the establishment of a Human Vaccine Production facility has kicked off in earnest with the development of an action plan and identification of physical facilities to host the plant.
A meeting between Health Cabinet Secretary Mutahi Kagwe and the committee on human vaccine manufacturing under the chair of the Kenya Medical Research Institute (KEMRI) on Monday reviewed the action plan for the establishment of the facility whose roll out will be implemented in three phases.
Also Read: Exploring how AfCFTA can avail cheaper medicines for Africa
Speaking at the meeting held at the new KEMSA facilities in Embakasi Nairobi, Kagwe said the government has already initiated discussions with vaccine manufacturers as Kenya seeks to build its own capacity for the production of human vaccines to ensure it becomes self-sufficient in its vaccine needs.
“There has been a lot of interest in this initiative by the Kenyan government. We need to remain on our path regardless of what comes up. In the next 12 months, we need to get this job done” said the CS.
The Health CS says the government is already engaging international partners involved in vaccine manufacturing to allow for technology transfer as it seeks to enhance the country’s capacity in the area of Research and Development.
How will this work?
The first phase of the project that includes setting up of basic infrastructure is on course with the identification of physical space within Kemsa premises in Embakasi set to host the fill and finish facility.
This phase, expected to be completed within a period of 9-12 months, will include refurbishment of the facility as well as the installation of the fill and finish line. The second phase, expected to cover a period of 18-24 months, will see the establishment of a full-fledged bulk antigen production facility. The third phase will revolve around capacity building with a focus on research and development and see the establishment of a vaccine/biological products research and development center.
“We have engaged substantially with Vaccine manufacturers, founders of SA Jansen Institute (Aspen) as well as with the government of South Africa, and they have expressed interest in working with us. We would be happy to work with Johnson and Johnson,” said CS Kagwe.
Kagwe took the chance to challenge the Kenya Medical Supplies Authority and the Kenya Medical Research Institute to be more proactive in addressing the health challenges facing the country noting that in matters health, time is of utmost essence.
“We must operate with a very futuristic approach. We must look into the future and see expansion possibilities and ensure that our projects are completed on time. As a Ministry, we must learn to work comprehensively with institutions collaborating and building on existing synergies,” said the CS.
The team presented the cabinet secretary with a concept note, budget, and selected portfolio of vaccines to be manufactured for approval within the next nine months. In anticipation of Kenya’s transition for support for childhood vaccines, the Technical Working Committee under the chairmanship of Lt. Colonel (Rtd) Dr. Daniel Mbinda who is also the board chair for Kemri, proposed consideration for immediate production of vaccines against polio, diphtheria, tetanus, pneumococcal pneumonia, rotavirus and hepatitis B which currently do not have patents.
Also Read: Private clinics in Africa to make billions from Covid-19 vaccines
The ministry will also be expected to establish a legal structure similar to KEVEVAPI to be called Kemri Biologics and Vaccines Institute (Kemri BioVac). It will also follow up with major vaccine manufacturers for partnership on technology transfer and supply of bulk Vaccines.
The Kenya Medical Supplies Authority is also working on enhancing its cold chain capacity to allow for storage of vaccines at temperatures of up to -80 degrees at its new godowns in Embakasi that are near completion.
The latest development comes in the wake of a biting global shortage of covid-19 vaccines occasioned by delays in delivery from Covax, a global coalition tasked with administering vaccines to lower- and middle-income countries. The shortage has slowed ongoing mass vaccination drives, especially across many African countries.
How can vaccine production be scaled up in Africa?
For Africa, according to WHO, focusing specifically on the technical aspects, what might work best is to establish what is called fill/finish capacity first otherwise referred to as drug product manufacture.
This would allow for collaboration with multiple partners for multiple products using a single formulation/filling line, it says.
Then in a phased approach step, back up the vaccine manufacturing value chain and install capacity to produce drug substance: antigen or active pharmaceutical ingredients. This is exactly the approach that Kenya is eyeing. This approach manages the investment risk upfront and builds vaccine manufacturing know-how in a manageable way.
The current COVID-19 pandemic presents a great opportunity to harness the various conversations and proposals into an action-oriented road map lead by the African Union and regional bodies that will lead to increased vaccine production in Africa to facilitate immunization of childhood diseases and control outbreaks of highly infectious pathogens.