Nearly 4.5 million Tanzanians in Dar es Salaam have received two drugs in a first step towards eliminating elephantiasis.
The disease is caused by Lymphatic Filariasis (LF) in Kenya, Uganda, and Tanzania. Towards its elimination, there were huge setbacks by Covid-19 restrictions and spending cuts.
Ending elephantiasis as a public health problem in the three nations would make them the first cluster of countries in Africa to achieve the breakthrough. This, following the announcement by the World Health Organisation (WHO) in January 2020 that Malawi had eliminated the disease as the second country in Africa, after Togo in 2017.
Read: Past and present poverty elimination efforts and existing potential in Tanzania
Elephantiasis, which is classified as a Neglected Tropical Disease (NTD), causes swelling and disfigurement and has left thousands of East Africans permanently disabled.
Kenya, Uganda and Tanzania were advancing rapidly towards eliminating the disease, until early 2020 when Covid-19 restrictions halted the preventative and curative drug treatments and surveys to assess the progress towards elimination.

However, rapid mapping of the new gaps in funding has now brought emergency funds, with the Children’s Investment Fund Foundation stepping in to finance Crown Agents to deliver the Dar es Salaam treatments, as well as mass drug administrations in Zanzibar and, for other Neglected Tropical Diseases, in Kenya and Uganda.
“The new CIFF funding for Kenya, Tanzania and Uganda has been essential in moving the dial on LF, from millions of people at risk to now very few. In this, the Dar es Salaam MDA is critical as a key measure in eliminating the disease in three of the last eight districts with LF in Tanzania,” said Deo Damas, Crown Agents’ Country Lead in Tanzania.
The emergency programme has not yet filled all the financing gaps, with planned surveys to detect the remaining prevalence now suspended as well as training and initiatives to treat NTDs under the countries’ universal healthcare programmes.
Read: Health SMEs still struggling for funding: finding
The UK government’s NTD programme, which accounted for a large part of the world’s spending on NTDs, was also due to funding the last 2,100 LF surgeries in Kenya, 2,500 in Uganda and 5,000 in Tanzania, to remove painful fluid sacs that are a feature of the disease.
Finishing these surgeries and putting in place case management for the thousands of citizens with incurable swelling are preconditions to achieving elimination under WHO criteria.
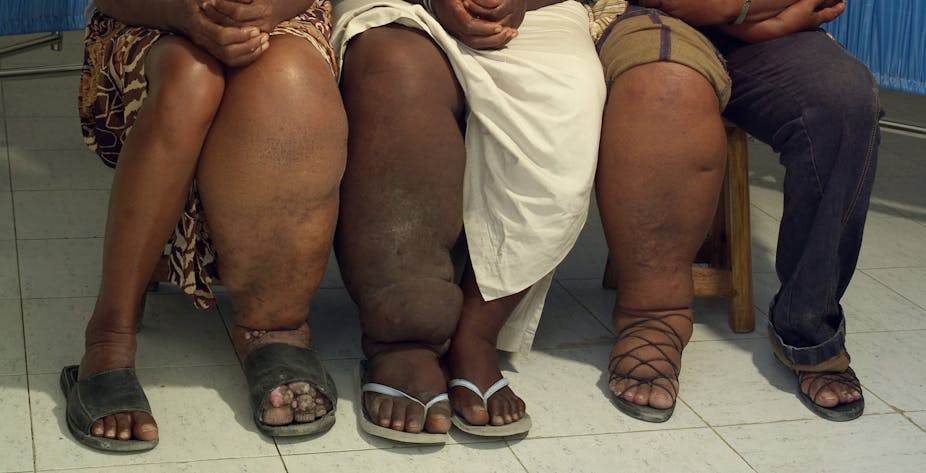
In Tanzania, where LF was endemic in 120 districts, repeated rounds of drug administrations have seen it eliminate the disease as a public health problem in 112 districts. The Mass Drug Administration in Dar es Salaam in recent days is the first of two rounds now due in three of the city’s districts as the country works to eliminate LF in its last eight districts.
Intense negotiations are now underway across East Africa to source funds for the final surgeries and assessment surveys to get the region to final elimination status.
“The progress in reducing the number of infections has been colossal, but now we need to pursue the countdown to elimination by raising awareness, clearing the last round of mass drug administrations, rolling out assessment surveys, and delivering surgeries and case management for those still suffering from the disease,” said Elodie Yard, the regional manager for Nairobi-based Oriole Global Health, which is managing the newly funded drug rounds in Tanzania and Kenya.
Read: More capacity building needed in the surgery ecosystem in Africa