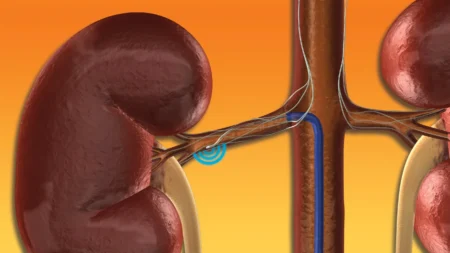
Kenya has been chosen to host the African events around antibiotic use with increasing concerns about the effects of the misuse of these vital remedies and the impact it is having on public health.
It is the first time for the Regional Tripartite, including the Food and Agriculture Organization of the United Nations (FAO), World Organisation for Animal Health (OIE), and World Health Organization (WHO), and the African Union, specifically Africa Center for Disease Prevention and Control (Africa CDC) and AU Interafrican Bureau for Animal Resources (AU-IBAR), to jointly organize the World Antibiotic Awareness Week.
Antimicrobial Resistance (AMR) is a major global threat of increasing concern to human and animal health. Antimicrobial resistance happens when microorganisms (such as bacteria, fungi, viruses, and parasites) change and become resistant to antimicrobial drugs (such as antibiotics) to which they were originally susceptible to. This can be due to different factors such as the misuse or overuse of antimicrobials and exposure to falsified drugs.
Microorganisms that develop resistance to the majority of commonly used antimicrobials are referred to as “superbugs”. The continued rise in antimicrobial resistance globally has led to 10 million people dying every year and will also account for 3 percent reduction in GDP by 2050.
Several institutes and groups of scientists have observed the negative impact the misuse of antibiotics have on the future of the health systems across the globe and have embarked on reversing these losses. For example, scientists have warned that as microbial resistance gains momentum, it will become extremely difficult to treat common ailments as the microorganisms will have evolved to levels where common antibiotics can not handle.
The burden, according to Dieter Schillinger, the Deputy Director at the Nairobi based International Livestock Research Institute (ILRI), is more on countries in the developing world that do not have established systems of monitoring and collating the effect the resistance has on small scale farmers as well as households.
He says the challenge with the resistance is the lack of available data to show the extent that it was affecting households in Africa.
The use of antibiotics cuts across from farms where farmers administer various lines of antibiotics and often in the wrong doses, either too little or too much. Sometimes, scientists have observed that antibiotics are retailed while combined with essential nutrients like vitamins or minerals.
Read also: Is Kenya the new entry point for the big pharma agenda?(Opens in a new browser tab)
In the health sector, self-medication as well as failure by patients to finish a dose. This leads to micro-organisms developing strength against medication making treating them harder and more expensive. According to Dr. Loice Achieng, a researcher at the University of Nairobi, over time, there has risen strains of bacterias that have grown increasingly hard to treat and at times, more expensive treatment regimens are imported to treat something that years ago would have been treated with penicillin.
Sam Kariuki is a researcher at the Kenya Medical Research Institute (KEMRI). Over the years, Kariuki and his team have looked at the correlation with the normal health challenges in the country. One of the observations the team at KEMRI was that unlike in the past, the emergence of cholera was becoming more pronounced and new outbreaks coming in drier times of the year unlike in the past. After various research endeavors, the team has found that cholera causing micro-organism was taking longer time in the environment beyond the treatment period hence become deadlier.
In collaborative research in various dump sites led by KEMRI, ILRI, Ministry of Health and the University of Liverpool observed that there was an easy move of micro-organisms from humans to animals with Nairobi dumpsites and rivers acting as a conveyor belt of Antimicrobial resistance.
Addressing the rising threat of AMR requires a holistic and multisectoral approach – referred to as One Health including public, animal, and environmental health. The cause and impact of AMR overarch all sectors.
ILRI is one of the entities that are coming up with strategies to counter the effect of AMR in the developing countries. The CGIAR Antimicrobial Resistance Hub, led by the International Livestock Research Institute (ILRI), applies a One Health approach to support the efforts of low- and middle-income countries (LMICs) in controlling agriculture-associated AMR risks, through promoting and facilitating transdisciplinary partnerships.
Read also: Kenya vet suppliers umbrella body to protect, promote interests(Opens in a new browser tab)
The recently adopted CGIAR AMR strategy recognizes the need for evidence on links between agriculture (crops, livestock, and aquaculture) and public health outcomes. Based on evidence generated, the hub develops solutions that are locally relevant and applicable, while being adaptable to other contexts.
Arshnee Modley, the new head of the CGIAR AMR hub in Nairobi notes that to counter the effects of AMR in developing countries requires joint efforts from farmers, drug manufacturers, animal feeds manufacturers and government agencies to ensure that the livestock sector is free from the resistance.
The Kenyan government recently announced plans to stop farmers from using animal manure unless treated. This was after fearing of bacteria like e-coli moving from animals to crops and specifically the lucrative export market. Allan Azegele works with the Department of Veterinary Services and acknowledges there are real fears in the movement of bacteria from animals to crops as well as the presence of chemical residues in the manure which in turn can be absorbed by crops.
Two years ago, the Kenyan government developed a Policy and National Action Plan aimed at reducing the burden of Antimicrobial Resistance (AMR) in the country.
The joint venture between the Ministries of Health and Agriculture, Livestock and Fisheries is using the one-health approach to promote prudent use of antimicrobial agents to ensure that there is continued successful treatment and prevention of microbial diseases by ensuring that effective, quality and safe antimicrobial are accessible to all who need them.