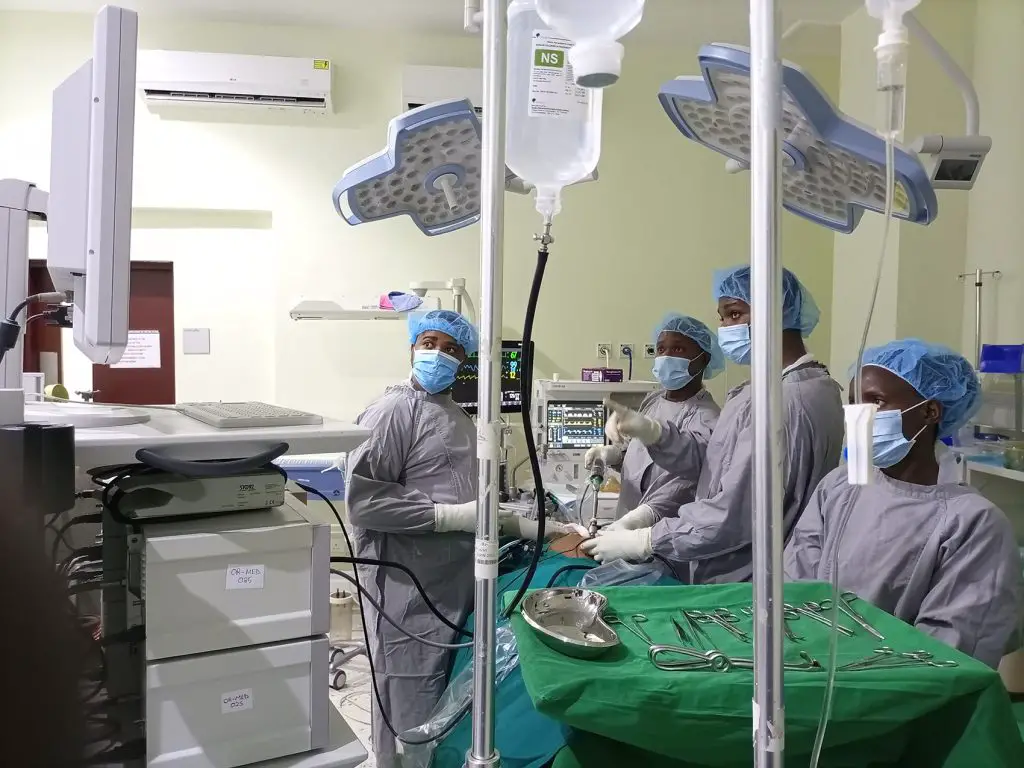
With more than 11 million confirmed cases and over 530,000 deaths globally, the COVID-19 pandemic continues to have a devastating impact around the world. While many countries continue to grapple with the ongoing surge of new cases, the pandemic has offered the opportunity to reflect on the current achievements and challenges of our healthcare systems.
For one, the novel coronavirus has created an unprecedented disruption for healthcare systems, which have had to balance between maintaining ongoing operations, scaling-up infectious disease programmes, supporting healthcare workers, and managing financial stress while supporting their communities. At an institutional level, the pandemic has forced our hospitals, clinics and other health institutions to quickly scale up their clinical, facility and support protocols to provide efficient and meaningful care to those in critical need.
But for health institutions, like Aga Khan Health Services (AKHS), the concept of pandemic response planning is not only built into our core infrastructure but is a necessity. As a network that operates at the grassroots, community level, an investment into pandemic preparedness has enabled the agency to respond to the current crisis in a well-coordinated and swift manner. In East Africa, for example, AKHS mobilised quickly to support government efforts to minimize the transmission of COVID-19, to prevent secondary outbreaks, and to ensure that our facilities are able to provide optimal care for those who are severly and critically ill.

AKDN / Aly Z. Ramji – The Exchange
To support this work, we monitored the global spread of COVID-19 to anticipate and plan for an influx of patients at our institutions; looking at everything from the number of additional beds required, the need to source a larger volume of essential medical supplies, such as ventilators; adapting requirements for key support services, such as housekeeping and food/nutrition services; and sourcing of a continuous supply of Personal Protective Equipment (PPE) to ensure hospital staff and volunteers are protected. The latter of these proved particularly difficult as hospitals, clinics and health institutions around the world grappled with the shared challenge of maintaining adequate amounts of PPEs to weather the crisis.
Also Read: Aga Khan hospital leads battle against Prostate Cancer in East and Central Africa
Despite this and other challenges that are inherent in the management of a pandemic, we – at AKHS – realised early that our greatest assets in this fight were our staff who dedicated their time, took great personal risk and worked exceedingly hard to provide the highest quality of care to our patients. As such, ensuring staff safety and building positive staff morale have become central to our mission.. We have focused our efforts on ensuring that our staff have the right support and resources in place, including ongoing training on evolving requirements and guidelines that impact hospital protocols, continuous monitoring of staff health to provide the care they may require as they continue to expose themselves to the virus through the course of their work, provision of psychosocial support and added support for their families who have equally taken on the risk of this pandemic.
Beyond staff relations, health institutions must also prioritise communications as a strategic imperative when dealing with a pandemic. An effective communications strategy is critical to ensuring the community is informed, prepared, and ready to act on preventive measures. Over a 12-week period, AKHS institutions in East Africa developed over 50 posters, 10 videos and hosted 13 on-line webinars to raise awareness about personal hygiene and physical distancing practices, as well as specialised subjects related to the effects of COVID-19, such as pregnancy, mental health, and child care.
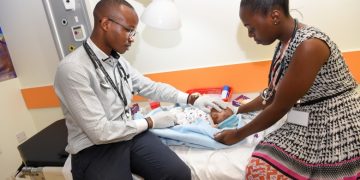
AKDN / Aly Z. Ramji – The Exchange
While the pandemic has been grossly destructive to societies around the world, it has also forced us to test digital innovations in our communities. AKHS’ use of virtual consultations (also known as telehealth or telemedicine services) during the pandemic has allowed the agency to provide patients with ongoing access to doctors and nurses without requiring them to come into our facilities.
This, coupled with the launch of the CoronaCheck mobile app (developed in partnership with Aga Khan University’s Technology Innovation Support Centre) has helped the agency advance its use of digital technologies to deliver healthcare. The app, which was launched in Tanzania in May 2020 and is available for download at no cost in the Google Play and Apple App Store, uses an interactive chatbot driven by Artificial Intelligence to help users understand their symptoms, recognise whether they may have contracted COVID-19 and seek medical care in a timely manner. It also aims to identify potential coronavirus carriers and limit their risk of transmission. To date, there have been over 12,000 downloads of the app in Tanzania alone and it is set to launch in Kenya in July.
Also Read: Aga Khan Building Capacity For E. Africa Healthcare Professionals

AKDN / Zahur Ramji
It’s clear that COVID-19 will change health care systems. While the long-term impacts of this pandemic are still to be determined, the following key trends warrant further discussion:
- Strengthening the continuum of care from the primary to tertiary levels, with strict adherence to the established national referral protocols is important. Patients need to be treated at the appropriate health facility and, if required, to move through the system seamlessly.
- Strong primary care with a cadre of trained community health workers who are grounded in the community can play an important role in disease prevention and surveillance and can help support the health system. The WHO-sponsored Astana conference of 2018 declared, “We are convinced that strengthening primary health care (PHC) is the most inclusive, effective and efficient approach to enhance people’s physical and mental health, as well as social well-being, and that PHC is a cornerstone of a sustainable health system for Universal Health Coverage (UHC) and health-related Sustainable Development Goals”. Well-developed primary care can play an important role in early diagnosis and proactive monitoring of patients, which will also reduce demand for hospital services.
- There will be accelerated use and mainstreaming of digital health. The COVID-19 pandemic is quickly transforming the acceptability of the use of digital health technologies. We will see an increased use of tele-monitoring, tele-diagnosis and tele-consultations in the months and years to come.
- Partnerships are essential. Effective and meaningful partnerships involving government and private health care providers will become even more important to pursue a collaborative effort in dealing with the post COVID-19 situation and any other disease outbreaks in the future. Partnerships and participation in joint planning and implementation structures will allow positive policy development, minimise duplication, and share resources in order to lead to the best possible outcomes.
By: Sulaiman Shahabuddin, Regional CEO, Aga Khan Health Services, East Africa
Aga Khan Health Services, East Africa
Providing high-quality health care and raising the health status of people in East Africa are the broad goals of the Aga Khan Development Network for the health sector. They are addressed through an emphasis, in current projects, on health systems development, strengthened by new regional programmes and investments.
The Aga Khan Health Services (AKHS) operate facilities in Kenya and Tanzania that provide health care to over 700,000 patients per year. An increasingly comprehensive range of high quality clinical services, both preventive and curative, are provided by their hospitals in both rural and urban contexts. In Tanzania, AKHS works closely with various stakeholders, including the Ministry of Health, to improve the health of vulnerable population groups, especially mothers and children, and promote health services development on the national and regional levels.
For more information please visit Aga Khan Health Services in East Africa